Navigating the keto flu and carb cravings: an expert guide for beginners
Understand the physiological mechanisms behind keto flu symptoms, discover evidence-based strategies for rapid relief, and learn how to conquer carb cravings during the transition to ketosis.
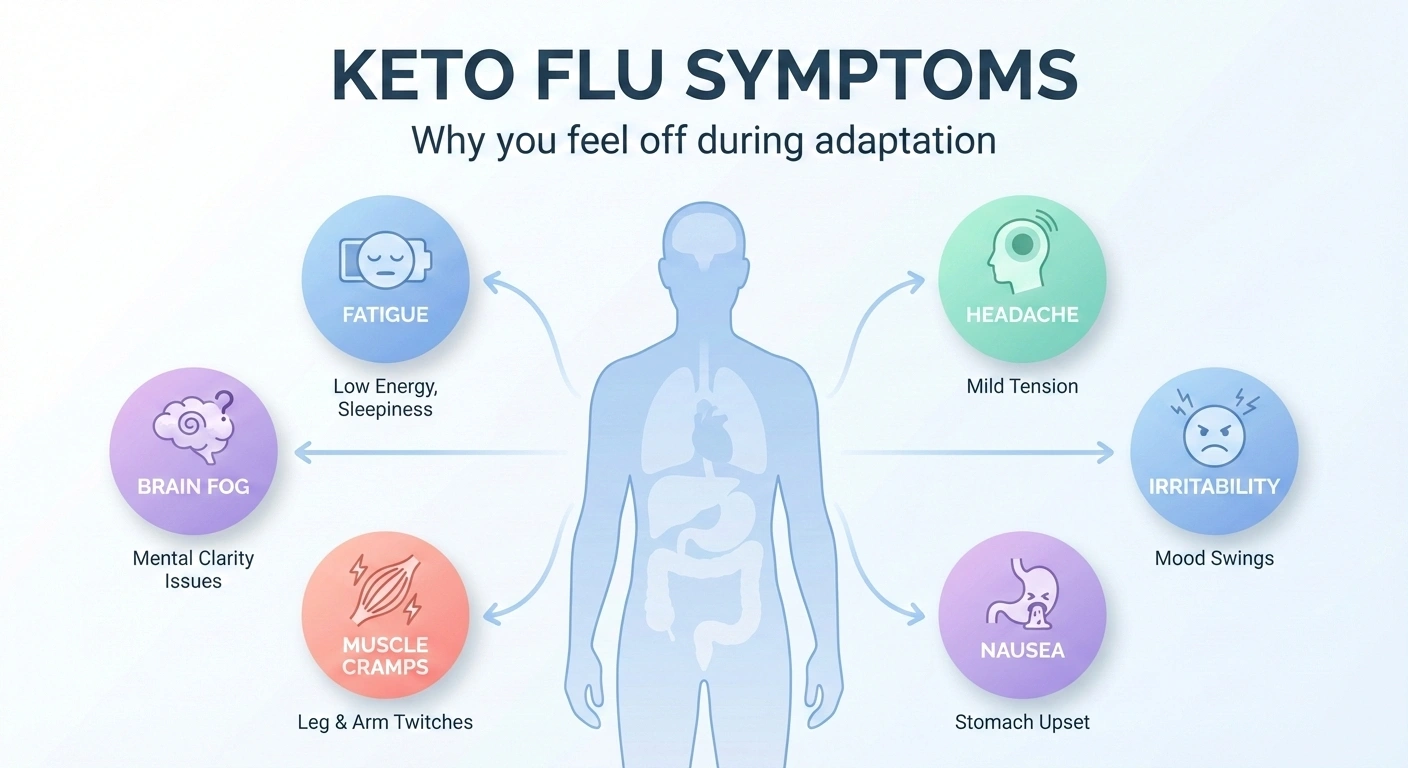
Overview: what is the keto flu?
Initiating a ketogenic diet — a nutritional approach characterized by very low carbohydrate intake, moderate protein, and high fat consumption — requires a profound metabolic shift. The body transitions from utilizing glucose as its primary energy source to producing and burning ketone bodies derived from fat, a state known as ketosis.
While this metabolic reprogramming is associated with potential benefits such as improved energy stability, mental clarity, and weight management, the initial transition phase can be challenging. A common consequence reported by individuals drastically reducing carbohydrate intake is the emergence of transient, flu-like symptoms — colloquially termed the keto flu (or carb flu). This guide provides an analytical overview of the underlying physiological mechanisms causing the keto flu and intense cravings, along with evidence-based strategies for mitigation and successful adaptation.
Understanding the metabolic shift: what causes the keto flu?
The keto flu is not a genuine infection. Rather, it represents the body’s reaction to carbohydrate restriction and the subsequent metabolic adjustment. When carbohydrate intake is severely reduced (typically below 50 grams per day), the body is forced to deplete its stored glucose (glycogen) and initiate fat burning (ketogenesis). During this transition — where the body struggles to efficiently use either glucose or ketones for fuel — temporary malaise occurs.
The role of electrolyte imbalance and dehydration
The most critical factor contributing to keto flu severity is the rapid loss of water and essential electrolytes — the primary driver behind most uncomfortable symptoms.
- Glycogen depletion and water loss: stored glycogen in cells retains a significant amount of water. When carbohydrate stores are depleted, this associated water is released and excreted through increased urination, causing rapid initial weight loss primarily from fluid volume reduction.
- Hormonal shifts and mineral excretion: restricting carbohydrates lowers circulating insulin. Lowered insulin signals the kidneys to excrete more sodium in the urine, along with potassium and water. This loss of crucial minerals — sodium, potassium, and magnesium — is believed to be the primary driver of keto flu symptoms. See our full keto electrolytes and hydration guide.
- Low blood pressure: the loss of sodium and the subsequent reduction in blood volume can lead to temporarily lower blood pressure, resulting in feelings of weakness, dizziness, or sluggishness.
Energy transition and glucose withdrawal
Prior to the keto diet, the body — and especially the brain — relies heavily on glucose for energy. When glucose is suddenly restricted, two issues arise:
- Temporary energy gap: it takes time (typically a few days to a week) for the liver to upregulate the necessary enzymes and fully adapt to producing ketones efficiently, and for the brain to learn to utilize ketones as fuel. During this learning curve, the body experiences a temporary energy deficit.
- Insulin resistance resolution: when tissues are accustomed to running on glucose, the reduction in blood sugar and insulin is a desired therapeutic outcome — but the temporary adjustment can cause lightheadedness and poor concentration as the brain transitions its fuel source.
Symptom presentation and duration of the keto flu
The symptoms associated with the keto flu can vary widely among individuals. Those who previously consumed a high-carb, high-sugar diet are more likely to experience more pronounced symptoms during the transition.
- Headache
- Dizziness, lightheadedness
- Poor concentration / brain fog
- General confusion
- Fatigue and exhaustion
- Irritability and mood swings
- Reduced motivation
- Trouble sleeping
- Muscle cramps or soreness
- General muscle weakness
- Nausea
- Constipation or diarrhea
- Heartburn
- Sugar/carb cravings
- Acetone-like breath (keto breath)
Typical Duration Timeline:
In more pronounced cases, symptoms may persist for up to two weeks. Aggressive electrolyte replenishment — particularly sodium — is the fastest way to shorten duration.

Clinical strategies for mitigating keto flu symptoms
Effective, straightforward measures exist to alleviate discomfort and support the body’s adaptation. These strategies primarily target hydration and electrolyte balance — the core root causes of keto flu symptoms.
Optimized fluid and sodium intake
Given that the rapid loss of water and sodium is the major contributor to keto flu symptoms, increasing the intake of both is the most crucial and fastest-acting intervention available.
- Increase water consumption: aim for a minimum of 2.5–3 liters of fluid daily, especially during the first week. Hydration helps relieve headaches and boosts energy levels by counteracting the fluid loss from glycogen depletion.
- Replenish sodium (salt): actively increasing salt intake replaces the sodium lost through accelerated kidney excretion. This simple action can often relieve symptoms like headache, lethargy, or nausea within 15–30 minutes.
- Practical sodium sources: stir half a teaspoon of salt into a glass of water, or drink 1–2 cups of bouillon, consommé, or bone broth daily. Bone broth provides electrolytes and trace minerals without carbohydrates. Beginners may need to increase their salt intake by 1–2 grams per day above their baseline.
- Potassium and magnesium: beyond sodium, ensure adequate intake of potassium (avocados, mushrooms, leafy greens) and magnesium (nuts, seeds, dark chocolate). Magnesium glycinate supplements specifically help alleviate muscle cramps and improve sleep quality during adaptation.
Strategic macronutrient adjustments
While it might seem counterintuitive for weight loss, adequate caloric and fat intake is critical during the adaptation phase to prevent worsening keto flu symptoms. Calculate your exact targets with the free keto macros calculator.
- Do not severely restrict calories simultaneously: focus on limiting carbohydrates (below 20–50g net carbs per day) but avoid aggressively restricting total calorie intake during the first 1–2 weeks. Trying to cut both calories and carbs at the same time exacerbates symptoms. Eat enough allowed foods until satiety is reached.
- Increase healthy fat consumption: fat is the new primary energy source. Consuming sufficient healthy fats — olive oil, avocado, grass-fed butter, fatty fish — helps fuel the body and speeds the transition to ketosis.
- Incorporate MCTs: MCT oil or MCT powder can rapidly boost ketone levels, reduce the time required to enter ketosis, and decrease keto flu symptoms. Start with a low dose (1/2–1 tablespoon) to avoid digestive discomfort, and increase gradually.
- Ensure adequate protein: moderate protein intake (typically 20–25% of calories, or 1.5–2g per kg body weight) is necessary for satiety and muscle preservation. See our guide on how much protein on keto.
- Prioritize fiber-rich vegetables: eating low-carb, high-fiber vegetables (leafy greens, broccoli, cauliflower, zucchini) is crucial for gut health, satiety, and replacing lost minerals — especially potassium and magnesium. See the keto vegetables list.
Managing physical and mental stressors
The metabolic adaptation process places temporary stress on the body. Reducing external stressors can significantly ease the transition and minimize the severity of keto flu.
- Prioritize rest and sleep: 7–9 hours of high-quality sleep per night is vital for hormonal balance and metabolic recovery. Poor sleep increases cortisol, which can inhibit ketone production and worsen symptoms. Reduce screen time before bed and avoid late-day caffeine.
- Avoid strenuous exercise: high-intensity interval training and heavy weightlifting should be minimized during the first 1–2 weeks, as they exacerbate fatigue and electrolyte depletion. Recommended light activities: walking, restorative yoga, stretching, light cycling, or swimming — these relieve muscle tension, boost mood, and help deplete glycogen stores faster without overtaxing the adapting metabolism.
- Manage stress: chronic stress increases cortisol levels, which stimulates glucose release into the blood — potentially blocking ketosis and intensifying symptoms. Incorporate stress-reducing activities: meditation, deep breathing, or journaling.
- Consider a gradual transition: for individuals experiencing debilitating symptoms, a slower reduction of carbohydrates over several days or weeks provides the body with more time for metabolic adaptation and may significantly reduce or eliminate keto flu entirely.

Conquering carb and sugar cravings on keto
Intense cravings for carbohydrates and sugar are common during the initial phase of dietary conversion, often coinciding with the keto flu. These cravings represent the body’s physiological demand for the glucose it is accustomed to — acting as a withdrawal symptom.
Physiological roots of cravings
Understanding the drivers behind cravings is key to managing them effectively.
- Blood sugar rollercoaster: refined carbohydrates cause rapid spikes and subsequent crashes in blood sugar, leading to cyclical hunger and intense cravings. The high-fat, low-carb nature of keto naturally stabilizes blood sugar over time, eliminating these dramatic fluctuations.
- Hunger hormones: ghrelin (“the hunger hormone”) regulates appetite and satiety. Poor sleep disrupts the balance of these hormones, increasing cravings. Once fat-adapted, ketones themselves exhibit appetite-suppressing effects that make cravings far less intense.
- Electrolyte deficiency mimicry: thirst resulting from dehydration and electrolyte loss is often misidentified by the brain as hunger or cravings for salty foods. Drink water first when any craving strikes.
Dietary interventions for satiety
- Maximize healthy fats and protein: every meal should contain sufficient healthy fats (avocados, olive oil, fatty fish) and moderate protein. These macronutrients promote long-lasting fullness and stabilize blood sugar. In early weeks, eating to satiety rather than restricting calories is the priority.
- Counter sweet cravings with savory: initial carbohydrate cravings often intertwine with a desire for salty foods. Counter these with pickles, olives, bacon, or cheese — satiating options that satisfy the craving without spiking insulin.
- Hydrate first: when a craving strikes, drink a large glass of water before anything else. This often eliminates the feeling entirely if it was in fact misplaced thirst or dehydration.
- Scheduled eating: eating at least three meals per day prevents extreme hunger, which triggers impulsive craving behavior. Beginners should avoid extended fasting periods until fully keto-adapted.
Keto-friendly substitutes for common cravings
- Sweet cravings: use low-carb sweeteners (erythritol, stevia, monk fruit) to achieve sweetness without blood sugar spikes. Indulge moderately in high-cocoa dark chocolate (85%+). Prepare keto fat bombs (coconut oil or nut butter based), or serve berries (strawberries, raspberries) with heavy cream.
- Salty or crunchy cravings: pork rinds (chicharrones), cheese crisps, nuts in moderation, or vegetable sticks all mimic the texture and salt hit of chips or pretzels.
- Comfort food replicas: cauliflower mash instead of mashed potatoes, zucchini noodles instead of pasta, and cauliflower rice instead of regular rice are effective low-carb swaps. See our keto recipes for more ideas.
Note: while artificial sweeteners are generally allowed on keto, excessive intake of certain sugar alcohols (maltitol, sorbitol) may still influence blood sugar or cause digestive upset. Monitor individual tolerance closely.
Addressing behavioral and environmental triggers
- Plan ahead (environmental control): remove high-carb items from your pantry and restock with approved keto foods. Prepare keto-friendly snacks — hard-boiled eggs, cheese, jerky, nuts — in advance. Avoid keeping trigger foods that historically lead to uncontrolled consumption.
- Manage stress and emotional triggers: stress, boredom, or emotional distress can trigger a desire for high-carb “comfort foods.” Engage in non-food activities when cravings occur: a walk, reading, or a hobby shifts the brain’s focus away from food.
- Mindful eating: eating slowly and mindfully allows proper recognition of actual hunger and satiety cues. Many episodes of craving are habitual or emotional, not driven by genuine physiological need.
- Light exercise: regular low-intensity movement like walking regulates appetite, reduces cortisol-driven cravings, and keeps the mind distracted from food obsession.

Supplements that support keto adaptation
While a nutritionally complete diet based on whole foods is the foundation of a successful ketogenic transition, certain supplements can help minimize keto flu side effects and accelerate adaptation.
- Electrolytes (sodium, potassium, magnesium): as discussed above, electrolyte supplementation is paramount. Commercial electrolyte mixes containing balanced ratios of all three minerals are particularly helpful. Magnesium glycinate specifically is recommended for muscle cramps and sleep quality — avoid magnesium oxide, which has poor absorption.
- MCT oil or MCT powder: medium-chain triglycerides are rapidly converted by the liver into ketones. MCT oil or powder helps increase blood ketone levels and may reduce the time required to achieve nutritional ketosis. Adding MCTs to coffee or smoothies can boost energy and suppress appetite. Start with a lower dose (1/2–1 tablespoon) to avoid stomach discomfort.
- Exogenous ketones (BHB): beta-hydroxybutyrate supplements provide ketone bodies directly. BHB consumption can acutely increase ketone levels in the blood, mimicking ketosis benefits (reduced hunger, improved energy) during the transition period. They are not a substitute for full metabolic adaptation.
- B vitamins and fiber: due to the restriction of traditionally fortified grain foods, monitoring B vitamin intake is important. Focus on dark leafy greens, eggs, and grass-fed meats. Adequate fiber from low-carb vegetables maintains healthy digestion and prevents constipation during adaptation.
Cold turkey vs. gradual transition: which approach is better?
The approach taken to carbohydrate restriction directly influences the onset and severity of the keto flu.
| Parameter | Cold Turkey (Abrupt) | Gradual Reduction |
|---|---|---|
| Approach | Immediately cut carbs to <20–50g/day | Reduce carbs slowly over days or weeks |
| Time to ketosis | Faster — 2–5 days | Slower — 1–3 weeks |
| Keto flu severity | Higher risk of pronounced symptoms | Reduced or eliminated symptoms |
| Best for | People who prefer a clean break and can manage short-term discomfort | Beginners with high prior carb intake or those sensitive to adaptation symptoms |
Regardless of the method chosen, remaining persistent with the dietary change is crucial for long-term success. The initial discomfort is temporary; the metabolic benefits of sustained ketosis are the goal.
When to consult a healthcare professional
While the keto flu is generally temporary and benign, persistent or severe symptoms warrant medical evaluation.
⚠️ Seek medical consultation if:
- Prolonged or debilitating symptoms: dizziness, confusion, or extreme fatigue lasting more than ten days, or symptoms that become actively painful.
- Serious gastrointestinal issues: persistent nausea, vomiting, or diarrhea increase the risk of severe dehydration and require physician evaluation.
- Pre-existing conditions: diabetes (especially type 1 or those on insulin/SGLT2 inhibitors), liver or pancreatic disease, kidney stones, or a history of eating disorders all require medical supervision before starting keto. See our keto and diabetes guide.
- Distinguishing symptoms from complications: a physician can differentiate temporary keto flu from more serious issues, including nutritional deficits or, rarely, ketoacidosis. Understand the distinction: ketosis vs. ketoacidosis.
Medical supervision is important for monitoring cholesterol and lipid levels during the diet. Registered dietitians can also assist in creating a nutritionally complete plan tailored to individual needs, ensuring micronutrient sufficiency during the adaptation period.
Conclusion: achieving sustainable keto adaptation
The initial phase of the ketogenic diet — marked by the keto flu and intense cravings — is a necessary, albeit temporary, physiological hurdle. This phase represents the body’s monumental effort to transition from being a sugar burner to a highly efficient fat burner, relying on ketones for energy.
The four core strategies — applied consistently:
- Hydration first: drink plenty of water (2.5–3L/day) to counteract accelerated fluid excretion.
- Electrolyte replenishment: aggressively replace lost sodium (via salt or bone broth) and ensure adequate potassium and magnesium through food and supplementation.
- Fuel adequately: eat enough healthy fats and protein to satisfy hunger and power the metabolic conversion — avoid premature calorie restriction.
- Prioritize rest: reduce strenuous physical activity and ensure 7–9 hours of quality sleep to minimize cortisol-driven interference with ketosis.
Cravings — driven by glucose withdrawal, habitual behavior, or simple dehydration — are best conquered through preparation, high-satiety foods, and psychological redirection. By consistently applying these clinical strategies and listening carefully to the body’s signals, the unpleasant symptoms of the keto flu will subside, paving the way for the long-term benefits of sustained ketosis. Patience and preparation are the essential tools for building a truly metabolically flexible lifestyle.
FAQ: keto flu and carb cravings — clinical answers
The most common questions beginners have about keto flu symptoms, duration, cravings management, and the safety of the adaptation phase — answered with clinical precision.
For most people, keto flu symptoms begin within 1–2 days of starting carb restriction, peak around day 3–5, and fully resolve within one week. In more pronounced cases — typically among those with very high prior carb intake — symptoms may persist for up to two weeks. Aggressive electrolyte replenishment, especially sodium, is the fastest way to shorten the duration. Symptoms lasting beyond 10 days warrant medical evaluation to rule out other causes.
The fastest relief comes from replenishing sodium. Drinking a glass of water with half a teaspoon of salt, or consuming 1–2 cups of bone broth or bouillon, can relieve headaches, nausea, and fatigue within 15–30 minutes. This works because sodium loss — driven by lower insulin levels signaling the kidneys to excrete more salt — is the primary mechanical cause of most keto flu symptoms. Alongside sodium, ensuring potassium and magnesium intake addresses the full electrolyte picture.
Intense carb cravings during the first 1–2 weeks are driven by multiple simultaneous factors: the brain’s deep dependency on glucose, the rapid blood sugar stabilization that creates a withdrawal-like effect, hormonal shifts in ghrelin (the primary hunger hormone), and dehydration that the brain often misinterprets as food hunger. These cravings are physiological, not a sign of weakness. Once fat-adapted — typically after 4–8 weeks — ketones themselves have appetite-suppressing properties that dramatically reduce cravings. Hydrating first, eating to satiety on fat and protein, and keeping trigger foods out of the house are the three most effective practical tools during this phase.
High-intensity exercise — HIIT, heavy weightlifting, long-distance running — should be avoided during the first 1–2 weeks of keto adaptation. Strenuous workouts exacerbate dehydration, deplete electrolytes faster, and worsen fatigue on an already stressed metabolism. However, light activity is not only safe but beneficial: walking, gentle yoga, stretching, and light cycling help deplete residual glycogen stores, support mood through endorphin release, and relieve muscle tension without overtaxing the system. Resume normal training intensity once keto flu symptoms have resolved.
The most evidence-supported supplements for keto flu are electrolyte blends (sodium, potassium, magnesium) — these directly address the root cause. Magnesium glycinate specifically is valuable for muscle cramps and sleep disruption; avoid magnesium oxide which has poor bioavailability. MCT oil or C8 powder genuinely accelerates ketone production and shortens the energy gap — but start slowly (1/2 teaspoon) to avoid GI distress. Exogenous BHB ketones can provide a temporary energy bridge but are not necessary for most people and are expensive. Multivitamins and B-complex supplements support micronutrient coverage when grains are eliminated. Products marketed as “keto diet pills” without clear electrolyte or MCT content are generally overhyped and not specifically helpful.
For most healthy individuals, the keto flu is not dangerous — it is temporary and self-resolving. However, you should stop the diet and seek medical attention if: symptoms persist beyond 10 days without improvement; you experience severe confusion, extreme dizziness, or chest palpitations; persistent vomiting or diarrhea is creating a risk of severe dehydration; or you have a pre-existing condition (type 1 diabetes, kidney disease, liver disease) that you did not discuss with a physician before starting. The keto flu should never cause symptoms as severe as actual influenza. If something feels seriously wrong — it may not be keto flu. A physician can differentiate adaptation symptoms from rarer complications including nutritional deficiency or, in at-risk populations, the onset of ketoacidosis.
Related resources & tools
Clinical breakdown of every keto flu symptom with specific electrolyte dosing protocols and timelines.
The complete guide to preventing dehydration and electrolyte imbalance on the ketogenic diet.
Understand the metabolic state you are adapting toward — and why it’s worth the initial discomfort.
Slipped up on carbs? This guide covers the fastest evidence-based strategies to re-enter ketosis.
Calculate your exact daily fat, protein, and carb targets — the foundation of a properly formulated keto diet.
Once adapted, combining IF with keto accelerates fat burning and further stabilizes appetite hormones.
Explore more keto flu & adaptation resources
For additional information on managing the transition and understanding symptoms, check out these expert external resources:
